I want to preface this post by saying it's mostly about questions, not answers. I've had many readers and acquaintances ask me about what's been going on at Virginia Mason Medical Center in Seattle.
The short answer is: “I don't know, other than anything I've read in the news.”
I don't have any inside connections at VMMC and I haven't talked to anybody there.
But, I've long had a lot of respect for the Lean journey at VMMC. I've only visited once, as part of an MIT alumni tour group, and I came away with a positive impression. I've met VMMC leaders at conferences, including their long-time CEO and Lean champion, Dr. Gary Kaplan.
I've been a fan of the books written about the VMMC Lean journey and I appreciate them sharing what they've done:

I've never had any formal business relationship with VMMC, but the only conflicts of interest to disclose are:
- Former COO Mike Rona wrote the foreword to the first edition of my book Lean Hospitals
- CEO Kaplan wrote introductory material to my book The Executive Guide to Healthcare Kaizen
So, what's the recent controversy?
Back in late June, we started seeing headlines like this:
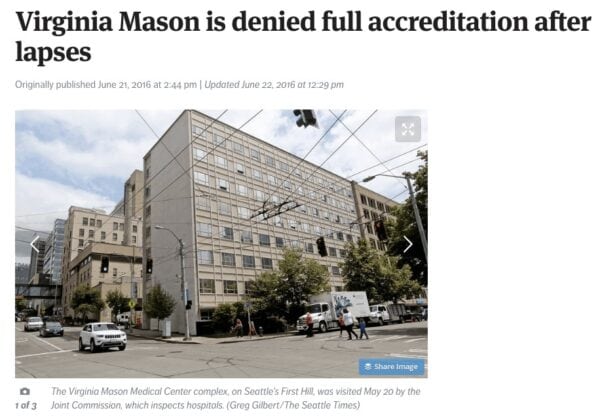
The “full accreditation” that was denied (or given provisionally) was from The Joint Commission, the main regulatory agency for American healthcare systems (and increasingly so throughout the world).
“Virginia Mason Medical Center in Seattle was found out of compliance in nearly 30 areas during a surprise visit in May by the Joint Commission, a nonprofit group that accredits hospitals across the nation.”
What were they out of compliance on? You can see the full list here. “The area is listed if one or more of the specific requirements were determined to require improvement.”
Update: the list of discrepancies is no longer online now that full accreditation has been granted after discrepancies were addressed
Some of the items include things that would be hard to believe are out of compliance for a hospital that has the reputation of having focused on operational details through Lean. The list includes things including (again, these were OUT of compliance):
- The hospital has an infection prevention and control plan.
- Before the hospital discharges or transfers a patient, it informs and educates the patient about his or her follow-up care, treatment, and services.
- The hospital safely stores medications.
- Label all medications, medication containers, and other solutions on and off the sterile field in perioperative and other procedural settings. Note: Medication containers include syringes, medicine cups, and basins.
That issue about labeling is especially surprising, considering the famous and tragic Mary McClinton story, where she died after an antiseptic from an unlabeled basin was mistakenly injected into her bloodstream in the cath lab. VMMC credits her story as a powerful motivator for patient safety improvement.
Their “last full survey date” at VMMC was October, 2014. So, did things backslide since then, in less than two years, or was the 2014 accreditation visit lacking in some way? There are many who complain about The Joint Commission visitors not always following the same standards or interpreting standards the same way.
It's also well known in healthcare that hospitals prepare for The Joint Commission visits by moving stuff out of hallways and creating a somewhat artificial environment to be inspected.
From the article:
“The Joint Commission conducts surveys every 18 months to three years, a spokeswoman said. The organization is the nation's oldest and largest accrediting body in health care.
At Virginia Mason, an unannounced follow-up survey will be conducted within three months to ensure that the deficiencies identified in the original report have been corrected, a Joint Commission document indicated.”
So, even though VMMC can correct the deficiencies and get full accreditation… but the headlines about any problems at a high-profile “Lean hospital” beings out the knives from the critics of Lean… those who claim Lean doesn't work in healthcare.
One of those places is in the politically-charged Canadian province of Saskatchewan, where VMMC's former consultant, John Black, was in the middle of a huge controversy over the past few years (read my blog posts on this).
The one headline was:
“American health facility using Lean fails accreditation“
“NDP health critic Danielle Chartier said she was concerned Virgina Mason was a “hallmark of the government's Lean learnings.”
She added she continues to hear from health-care workers with Lean-related concerns in the health-care system.
“The reality is, Lean is a tool in the tool box, but you don't use the same tool for every job,” she said.
The province spent $33 million on a contract with U.S consultant John Black to implement Lean.
Black was brought in to make the health-care system more efficient. It quickly became a favourite point of criticism for the NDP. In 2014, the government announced it was ending the controversial contract with John Black earlier than originally agreed.”
The Virginia Mason Institute (the training and consulting arm of VMMC) has been doing work in the British National Health Service (NHS) hospitals and there has also been some controversy and headlines trumpeting the problems at VMMC:
“Veteran health campaigner John Lister said it was “astonishing” that Mr Hunt ever “thought the lavishly-funded – and now evidently not very good – Virginia Mason could be in any way compared with the NHS”.
…
A spokeswoman for the National Health Action party, set up by doctors, nurses and paramedics in opposition to the Government's health policy, said the report proved the NHS should not be “copying” hospitals in the US.
She said: “The US system is a failing system being brought wholesale into the NHS.
“International comparisons have shown the NHS public service model of care to be a world leader at very low cost. The US system as a whole, not just Virginia Mason, is acknowledged as failing very many of its people and it is very costly.”
There are, in Canada and England, concerns raised about Lean and the “American-ization” of their hospitals. Lean, of course, is about improving healthcare delivery – processes and value streams – not turning anything into an American system (or a Japanese system, for that matter).
Does Accreditation = Safety?
Now, if VMMC critics say that not getting full accreditation immediately means the hospital is failing and isn't a model, does that mean hospitals that GET accreditation are safe?
Hardly?
Case in point is a Kentucky health system discussed here:
State investigates KentuckyOne hospital over staff layoffs
As also reported here in the local press:
“Dr. J. David Richardson, a prominent surgeon and current president of the American College of Surgeons, said cuts in nursing and other staff had caused a “major patient safety issue” and were “destroying the hospital.”
It must be pretty bad for a surgeon to speak out like that… and again, from Modern Healthcare:
“The Joint Commission re-accredited the hospital in January 2016 but did recommend it make improvements such as better documentation of infection prevention procedures.”
What's the difference between “failing accreditation” and getting accreditation with the recommendation of making improvements that sound very similar to what needed to be fixed at VMMC?
“Those included problems with infection prevention and transfusion errors as well as in broader categories, such as “the hospital plans the patient's care” and “the hospital effectively manages its programs, services, sites, or departments.””
Keep in mind The Joint Commission accredits most hospitals, yet we still have a huge patient safety crisis in the U.S. (see the various statistics).
But, VMMC Wins Many Awards
So, is Virginia Mason Medical Center a big mess?
Well, they were named one of the “Hospitals of the Decade” by Leapfrog Group, a leading patient safety advocacy group (conflict of interest disclosure: Leapfrog paid me to speak at one of their events in 2015 and I interviewed their CEO Leah Binder).
Leapfrog's “Hospital Safety Score” gives VMMC an “A” grade as of Spring 2016, based on a lot of data:

The recently released (and somewhat controversial) “star ratings” from CMS give VMMC a 4-star rating out of five, based on 64 different measures:

And yesterday, VMMC trumpeted the most recent US News & World Report rankings:
As my friend Paul Levy, a former hospital CEO, has pointed out the U.S. News rankings give a lot of weight to a hospital's “reputation” score, which seems like self-fulfilling prophecy. The best-known hospitals aren't necessarily the safest, if you look at the CMS or Leapfrog rankings.
You can see a summary of independent quality reports on the VMMC website.
So, what's the impact of The Joint Commission situation at Virginia Mason?
Does it mean there are serious problems and they shouldn't be considered a leading “Lean hospital” to learn from and emulate (but not copy from).
Or, does is it just a blip and a hiccup that hurts their reputation a bit and, possibly, hurts the reputation of Lean in healthcare?
What do you think? Are the headlines about Virginia Mason overblown? If you want to leave a comment, you can do so anonymously or contact me through this form anonymously.









I’ve only been with one hospital through the accreditation process, but from my conversations with others, this is highly unusual to have such a reputable hospital miss their full credentialing. It would be considered an epic fail for us if we had that many citations from our own survey. It is *definitely* not the norm.
My instinctive reaction is that this kind of thing is a crisis of leadership, pure and simple. There shouldn’t be many surprises about a JC survey, so a failure to meet that many requirements, even with a team of picky surveyors, means someone wasn’t minding the till, as it were. It takes enormous organizational energy to be survey-ready. I’ve never seen us do it with less than a VP-level person hounding it for months on end as the survey window closes and holding the entire leadership accountable.
The reason this is so interesting to me is that I’ve been working under a results-oriented senior team. The end goal is not to be a “Lean” organization, the goal is to be a top decile performing organization. Lean has been selected as a good methodology to help move us in the right direction. Our benchmarking models are not the most advanced lean hospital systems like ThedaCare and VMMC, they are the “Everest” Hospitals – the ones in the top tier of the “Top 100”. Only a couple of which practice Lean.
So is it that Lean is helpful but insufficient for excellent performance or that less than excellent performance just means a poor or immature implementation of lean?
I guess without more inside information, any discussion about VMMC will be wildly speculative. But the question you raised about the connection between accreditation and safety is an excellent one and is part of a different conversation.
I think you could say that an accredited organization has a basic floor of safety, but that’s probably as far as I would go. Still, I have become more grateful for that floor of safety after visits to third world hospitals without even that floor. For all its problems I’d rather live in a world with TJC than without.
To the excellent question about whether Lean is sufficient for excellence… I think it depends on the definition of Lean.
If Lean is viewed as a series of Rapid Process Improvement Workshops and staff-driven continuous improvement… or as a set of tools and methods, then Lean wouldn’t be sufficient.
There’s the vitally important management system and culture of Lean. This includes the nuts-and-bolts management of processes and people on a daily basis. Do people have enough time to do the work the right way? Are supervisors checking to see if standardized work is being followed (and if it CAN be followed)?
There’s a level of process discipline that’s supposed to come with a truly Lean culture.
It would be shame if VMMC wasn’t doing that… or if they lost some discipline over time (as has happened even at Toyota).
It would also be a shame if TJC was nitpicky or had an agenda, as Bart implied in his comment below…
In defense of VMMC, I believe they were probably in the cross-hairs of TJC due to the number of VMMC patient deaths associated with endoscope contamination over the past couple of years even though the deaths were attributed to the design of the scopes and not a lack of compliance with disinfection standards.
The recent failed survey shouldn’t take away from other excellent and notable improvements VMMC has made over past 15 years as a result of their Lean efforts.
On the other hand, based on a visit there several years ago, I went away with the impression that their efforts were heavily reliant on their improvement group as compared with their leadership team. I am not saying that leadership at VMMC is not involved in Lean efforts; clearly Gary Kaplan is. I am just saying that it wasn’t obvious to me that leadership had a significant role in front line improvement.
The other point is that Lean as taught and generally practiced at most healthcare institutions is based on a Lean production model. For all the talk about Lean being a management system my observation is that in application it is most often a collection of tools that can significantly improve various aspects of hospital operations. I think that this is evidenced by very few hospitals that have committed to Lean, or even attempted Lean, have abandoned their efforts. Hospitals have many moving parts and existing management systems, like TJC accreditation (an aspect of quality control), that most Lean efforts tend to ignore and where production models don’t apply or are late to reach.
A quick test to demonstrate this is to evaluate how senior leaders solve strategic problems. Do they jump to Lean tools? Do they attempt so solve problems by intuition or reflex? Do they delegate to underlings? Or, do they methodically try to understand the root causes, system issues, and pull together the best minds and stakeholders throughout the organization? So if your management system doesn’t impact how your senior leaders manage challenges then I posit that it is not a complete management system. There are some obvious Lean healthcare organizations where this is done, but it probably is a very short list and just because your organization has written a book about their Lean journey doesn’t mean that they aren’t open to the types of problems VMMC has.
Why would VMMC be “in the cross hairs?” That suggests a level of subjectivity or politics from the Joint Commission that I wouldn’t be comfortable with.
To your question about leaders… I’d hope they would practice what they preach about creating an environment where people are safe to speak up and point out problems. Does this occur not just in the operating room before surgery, but every day, everywhere? How many staff members were possibly trying to “pull the andon cord” about the issues that got them dinged by the Joint Commission (and, more importantly, could have been compromising safety)? VMMC has a “Patient Safety Alert” system… was that being invoked? Were leaders dismissive or slow to respond?
There’s more than just “Lean tools” for leaders to consider… what are their Lean mindsets and Lean behaviors? Do they share the Lean philosophy that helps create a truly Lean culture?
anonymous, A V-P level person hounding us for months….. there is a basic social system model that speaks to the Required System and the Emergent System.
Appears that Management in this hospital has made a conscious decision to run most of the time to operate in the Emergent System rather than in the Required System(TJC). Sort of like inner city schools that spend the semester teaching the test rather than the curriculum.
Dr Deming might be moved to ask “what is the purpose of your system?”
It’s a fair question — is working to pass TJC a matter of “teaching to the test?” It’s required for CMS reimbursement, but does it REALLY improve quality?
There is a TJC alternative, DNV, now.
TJC had a Congress-appointed monopoly on this accreditation game…
This is an interesting read: “Hospital administrators are scared of JCAHO”
http://www.kevinmd.com/blog/2013/11/hospital-administrators-scared-jcaho.html
JCAHO (The Joint Commission, don’t call them JCAHO) requires diversity training??? Does that help improve quality and patient safety?
“Hospital administrators are scared of JCAHO and would move heaven and earth, murder pets and children, desecrate holy ground, beat themselves over their heads with the jawbone of their ass, and sacrifice their finest sheep on the altar of bureaucracy in an attempt to avoid getting dinged for minor infractions during a JCAHO inspection.”
But Virginia Mason wasn’t scared of them?
Jack ,can we bring it down to where the Rubber meets the road from the perspective of the PATIENT : the poor helpless soul that provides the economic means ( the sand in the sand box within witch all these God like creatures play in. Why is this non descript person,who has no choice but to SUBMIT their body in to the 4 wall’s of the hospital.So what are the people that populate the hospital doing treating that helpless human being as an in convince to what the management of the system demands from the workers in the system .Adhereance to the annual and quarterly financial results.
In this era of “Fake News”maybe some level of management at Virginia mason can confirm whether this news is true or not,if it is can we have the £12.5 mil that the British government has paid to a company that proclaims efficiency in its sales pitch but displays sloppiness ,back.
God save the NHS .
Read the news articles I linked to. Not “fake news.”
Thanks Mark,Having lived in America for two years in the 70s its a country I have a great affectation for ,but one bit of advice an old American told me ,”When you are dealing with Yanks buddy,first and foremost they are all salesman”,I think in this case Virginia Masons dealings with our NHS, first and foremost they were all salesman.
God Save the NHS from snake oil peddlers
Mike, thanks. I appreciate that you’re not calling all Americans “snake oil peddlers.”
Why are you saying that about the Virginia Mason Institute? That’s quite a charge. Can you please explain more rather than just throwing insults at them?
Far from it Mark like I said America and Americans are a country and people I have a great respect and affection for but the kind of culture Virginia Mason seem to have are at total odds with the culture of our NHS which is a free at source cradle to the grave service funded by the tax payer ,and has been proved to be possibly the most cost effective and efficient health services ,how can VMI come to the UK after failing so badly giving expensive advice and expect us Brits to keep a straight face.
Fight the Good Fight
Mike
OK. You’re being very vague. How is the VM culture different in your view? “Snake oil” is a very serious and loaded term. I wish you could better explain what the issue is.
Maybe Snake Oil means something different in the States Mark, here it means your a top salesman ,according to the Commonwealth Fund of Washington DC The UKs National Health Service ranked first in quality and value for money but maybe this is “fake news”,like I said in my original question as I understand they failed an inspection by the US Government but maybe this is fake news ,maybe you could confirm if its true or not,as a UK Taxpayer I would hate to think we are not getting value for money.
Here is the common meaning here in the US:
https://en.m.wikipedia.org/wiki/Snake_oil
It means fraudulent. “Snake oil” means a tonic or medicine that doesn’t deliver any real value.
So maybe you understand my pushback on the term snake oil. You might disagree with their approach or have concerns. They might not be perfect. But that doesn’t mean hey are intentionally fraudulent.
Thanks Mark for that info.over here it means your a top salesman and they say we speak the same language,
Im still confused if the reports about VMI are fake news or not or if the Commonwealth Fund of Washington DC are a reliable source and “if”the reports are true why a National Health Service that was rated the best in the world by The Commonwealth Fund should pay a organisation that may or may not have failed an inspection by the US Government £12.5mil.for consultants fees .
It is true,seemingly The Virginia Mason Institute did fail an inspection by the USA Government ,also now The Optum Group has been given a contract by the NHS and “If its not Fake News”are being dragged through the American Courts for various failures,meanwhile we have President Trump making disparaging remarks about the United Kingdoms health service today ,assuming its not “fake news.
The inspection was by an organization called “The Joint Commission.” Calling them the “USA Government” is not accurate, speaking of “fake news.”
Just a thought ,If “Lean Medicine Theory”is based on the Toyota Lean Car Production Theory did not Toyota have to recall 11.5 million cars last year ,the difference being, I suppose that a car produced using Lean Car Production Theory can be recalled,more difficult with a hospital patient.
True. But also true is that far more people were killed by preventable errors in hospitals last year than were injured by defective cars.
Interesting dialog. I was hoping to see VMMC during one of our visits with our grandchild in Seattle. CORONA sort of put that on hold. I’ll still follow-up later. I’ve seen a couple of organizations that at one time were highly effective at improving…for many years. But as time goes by a complacency seems to settle in (my hypothesis based on a few observations…not yet validated with data). They still do a decent job with the tools, but the critical thinking, the sense of urgency that existed in the earlier years slows down. There is an assumption by the leadership team that they are still highly effective….but in daily practice, management is no longer quite as engaged, quite as passionate. Sometimes it takes outside eyes to look and see what is really going-on. Hopefully VMMC can regroup (assuming that is necessary) and reinvigorate what I thought was a highly effective organization.