Every time I am in a hospital or clinic setting, one of the first things I do is get a pump or squirt of gel or foam from a wall-mounted dispenser to clean my hands.
Or, I should say *try* to get hand sanitizer. For one, it's important to practice proper hand hygiene when entering or leaving a unit, for my sake and the patients (and to practice what I preach, a secondary concern). Secondly, I'm testing to see if the hospital's support processes work well – is the dispenser actually not empty?
It's usually not difficult at all to find an empty gel or foam dispenser on the wall. Sometimes, the first one I try is empty (as are others). Sometimes, I have to try a few… but there's almost always an empty one.
Staff Members Know This Problem Exists
Below is pictured a “Kaizen card” that one of my clients filled out in a nursing unit, identifying this as one of the first problems they wanted to tackle. You can actually see two two cards since it was that noticeable of an issue that staff noticed.

Before having an active and effective Kaizen process for continuous improvement, staff might just sigh and roll their eyes when the dispenser is empty.
If the dispenser is empty, a healthcare professional or visitor COULD walk to a different dispenser, but that's taking more time out of their already-busy day and if we don't make it super easy to practice hand hygiene, people are less likely to do it. They might make excuses like, “Well, I'm not going to touch the patient, so I'll just go in,” but staff often end up touching the patient, which could spread germs.
The connections between proper hand hygiene and patient infection rates are not a big mystery or secret at this point. This article described a patient who died from an antibiotic-resistant staph infection, MRSA, after a knee replacement surgery.
“When something happens like that, you get a hospital's acquired infection, the hospital staff will tell you, ‘Well, there's nothing we can do,'” Peters said.
…
Some hospitals, though, have dramatically improved their [safety] scores by using simple but stringent protocols, for policies and practices as basic as hand-washing. Some facilities have even driven infection rates down to zero.
Yet, this still haunts [the victim's daughter] Bimbaum to this day.
“The hand sanitizer outside his room was empty,” she said. “Meant to keep hands clean? Right.”
There's clearly SOMETHING that hospitals can do to make sure the dispensers aren't empty. This isn't rocket science.
Listen to Mark Graban read this post (learn more and subscribe):
Signs Haven't Solved This Problem
In attempts to “solve” this problem of poor hand hygiene, hospitals love hanging signs that lecture employees about proper hand hygiene. If those signs were really effective, we'd have already seen 100% hand hygiene adherence rates. But, they don't work.
On top of that, patients are told to ask nurses and physicians if they've cleaned their hands properly (see my site www.AskMeIf.com for more about this and why I think that's ridiculous and ineffective).
One hospital sign (as I shared at my site BeMoreCareful.com):

All of this browbeating does no good if the dispensers are empty.
Nobody ever hangs a sign that says:

Signs don't help. Instead of more signs, we need better systems and processes.
Since the foam and gel is a pretty critical supply that's needed for safe patient care, the hospital has an OBLIGATION to ensure that it's always available… unless there's a nation-wide shortage or something, but that's never the case. It's just an inattention to detail and poor processes. We can't “hold a person accountable” (or blame them) – we have to fix the system.
Toyota Has Great Systems & Processes
Toyota, our Lean luminary example, has excellent systems in place in their factories to ensure that production team members always have what they need to build cars and trucks. It's not that difficult to create the systems if you put the effort into it. Hospitals just need to focus on designing a better system and making sure they aren't shortchanging the number of support staff that are needed to refill these dispensers.
Toyota has an army of support people driving carts and pushing parts around their factories. They aren't “cutting costs” by mindlessly reducing the number of needed support staff. It's not just Toyota… all of the automakers probably have, at this point, equally precise and effective Lean materials management processes.
Ok, enough glorification of Toyota… in a hospital, dispensers look like this:
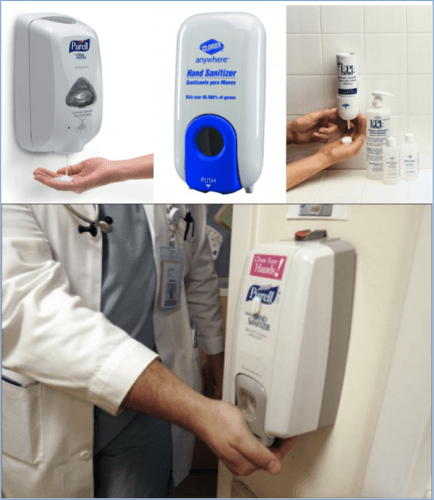
That bottom one even has an integrated “Clean Your Hands!” sticker (in pink). I guess that counts as innovation in this domain, putting the reminder or sign right on the dispenser?
Sometimes, the dispensers have a red flag on top (you can see it above the pink sticker in the photo there). If the dispenser is empty, you're supposed to put up the red flag as a signal that it needs replenished.
You might think, “Oh, good! Visual management! That's Lean!”
Well, what happens if nobody puts up that red flag? Empty dispensers often have the red flag in the down position. Should we invest in fancy technology that automatically raises the red flag or sends a wireless signal to somebody when a dispenser is empty? That's probably not necessary.
Again, I think it's the HOSPITAL's responsibility to provide sanitizer.
What's my idea for fixing it? It's a relatively cheap solution that doesn't involve electronics, RFID tags, or the like.
I call it the “two-bin dispenser.”
The Two-Bin System
It would be really super simple to solve this. But first, here's the silly inspiration for my invention.
Most places do a far better job of not letting a toilet stall run out of toilet paper. That's something we can all be thankful (although I'm sure many of you have a horror story about TP running out).
One way they ensure it doesn't run out is… a two-roll dispenser. Of course, they need to make sure the housekeeping staff comes around at the right frequency to restock the paper. Two empty rolls is no better than one empty roll.
The two-roll system is brilliantly simple. It's sort of like a “two-bin kanban system” that I've helped a lot of hospitals set up. When one bin is empty, you have a second bin (or roll) to use while you're waiting on restocking to take place. The worst thing that could happen is both rolls being used simultaneously so they're both empty at the same time, as would be possible with this type of dispenser.
Here's an example of an effective hospital lab two-bin kanban supply system:

Notice how the bottom bins are turned around backward. Why is that? That's a bit of clever error proofing that prevents people from using supplies from both the top bin and the bottom bin at the same time. When the top bin is empty, it's removed, which becomes the signal to replenish more. The bottom bin gets turned around and is now the one being used. If people took items from both the top and bottom bins, they might both be empty at the same time…
The size of the bins (or the toilet paper rolls) has to correspond to the frequency of the person who's coming around and checking the kanban bins. You can either adjust the size of the bin or adjust the frequency of the replenishment route to make sure everything works.
If that person comes daily to check for empty bins and then comes back the next day with a newly-full bin (if needed), each bin has to hold at least two days' worth of supply (and probably more… what's the MOST you'd expect to use in a two-day cycle?). If the person comes by weekly, you'd need to keep a week's worth of supply in each bin.
There's a pretty clear tradeoff between delivery route frequency and the size of those bins. More frequent delivery = small bins being needed. If you have a fixed-size bin, you might need to change the frequency of routes.
The Two-Bin Sanitizer Dispenser
So, here's my “invention” (but if this already exists, please leave a comment and let me know).
A simple two-bin sanitizer dispenser could be two dispensers inside a case, as I've crudely mocked up here. Instead of one dispenser, you'd need two. They could hang above and below each other.

Both dispensers start out full, inside this box or case that's hanging on the wall. People would use gel from the dispenser on the left (and only that dispenser). When it gets empty, you'd slide the plexiglass cover over to the left (and maybe put up a red flag?).

You now have a visual replenishment signal that's more useful because you still have sanitizer to use in the second dispenser.
This same idea could be implemented by having ONE dispenser that has TWO bags inside and maybe the pump button would need to have a left and a right side that pressed independently. When the left bag is empty, you slide over a switch that unlocks the right side of the single dispenser.
An approach like this, the double dispensers, would take up more space and there would be higher cost. But, this dispenser, combined with a properly-designed replenishment cycle, could completely eliminate the problem of empty dispensers. And, more importantly, it would increase hand hygiene adherence rates, would reduce infections, and would save lives.
Who is willing to make this happen? I'm not filing for a patent. Steal the idea. Run with it. Let me know if I can help you design a better replenishment process to use with it, because, again, two empty dispensers don't help any more than one empty dispenser.
Please scroll down (or click) to post a comment. Connect with me on LinkedIn.
Let’s work together to build a culture of continuous improvement and psychological safety. If you're a leader looking to create lasting change—not just projects—I help organizations:
- Engage people at all levels in sustainable improvement
- Shift from fear of mistakes to learning from them
- Apply Lean thinking in practical, people-centered ways
Interested in coaching or a keynote talk? Let’s start a conversation.









![When Was the Last Time a Leader Around You Admitted They Were Wrong? [Poll]](https://www.leanblog.org/wp-content/uploads/2025/07/Lean-Blog-Post-Cover-Image-2025-07-01T212509.843-100x75.jpg)
Awesome Mark. . . This needs to happen in bathrooms everywhere. Come on manufacturers! Gojo are you there?
Nice. Doing something like this for general soap dispensers would be welcome too.
Nice idea Mark. I’m in healthcare and I see empty dispensers all the time.
Building on your “invention” ;) we could have gel bags half the size of the dispenser and in this way you can load 2 inside, and the housekeeper would change and replenish when one is empty, just like the 2 TP system!
Mark-this is a great idea! As the leader in the Environmental Services department, we are hard pressed to keep all of the dispensers full. I am going to reach out to my hand hygiene vendor and find out if they have this in development, and if not suggest it!
Thanks, Kathy. I appreciate you doing that. I sincerely do hope this blog post helps bring about some change…
Mark,
I might suggest a different countermeasure (although I’m not as familiar with the sanitizer dispensers as you). I would create a simple two-bin system with visual management:
Keep the same dispenser that you currently have (either gel or the foam canister). Next to (or above) the dispenser, mount a small wire/plastic rack (inexpensive-already available) and place one replacement pack inside of the rack.
Now, when the dispenser is empty, any person can remove the empty bag/canister and replace it with the full bag/canister (simplifying “changeover” if needed). Kanban Rule: Just throw away the empty bag/canister in the trashcan when you enter the room.
Waterspider/facilities crew would replace sanitizer in any empty wire rack – the signal that replacement was needed.
I’m enjoying your audioblog – thanks for getting your stuff out there!
I like that idea… there are definitely different ways to solve this problem.
My concern with the “anybody refills it” part of the process is that “anybody” quickly becomes “nobody.” I’m not sure how long it takes to change out a bag, but it might take too long for a busy nurse. I’d still prefer somebody on a route who is checking and refilling the dispensers and that person could do the refill and then replace the “spare” bag that’s there).
Your approach would probably cost less, which is a very important consideration. There would just have to be a good process to make sure that the empty container doesn’t sit there with the “spare” bag also just sitting there unusable.
We’d have to test these ideas in a PDSA approach to see what works or doesn’t work.
I’m glad you like the audio blog!
I agree that signs don’t work well, but those ones IN PARTICULAR won’t work.
Why?
THE HUMAN EYE HAS MORE TROUBLE READING ALL CAPS THAN IT DOES READING CAPS AND LOWER CASE… AND THE CRUCIAL INFO IN BOTH THOSE SIGNS IS IN ALL CAPS.
And don’t get me started on the clip art.
Let’s take a card from Steve Jobs’ approach to design:
”[Design is] not just what it looks like and feels like. Design is how it works” – – Steve Jobs
Design has to go hand-in-hand with process.
Yeah, those signs are terrible… particularly bad. But, I’ve seen lots of better looking signs that seem to be just as ineffective.
I think a Steve Jobs approach would be to make the hospital functional, intuitive, and easy to use. And that, to me, means making sure the dispensers are full and not cluttering up your hospital with signs.
BRILLIANT! Coming from a Process Improvement dept at a hospital and witnessing First hand multiple ’empty’ hand sanitizer holders on the wall because so & so forgot to fill it or that’s is not my dept’s responsibility to refill. I Love this idea/concept. Thanks for sharing. Of course IF process owners relied more on accountability maybe less empty bins would be out there and the need for such product would not exist. Since there is an underlying root cause – lack of staff? Lack of accountability? Lack of understanding roles/responsibilities? For now experiencing the frustration of empty hand sanitizers I stick with Brilliant idea!!
I”m glad you love the idea. Thanks. But let’s discuss the process side…
“Lack of accountability,” to me, is in the same category of the statement “lack of staff motivation” that appears in the comment below.
If you’re in a process department, I’d implore you to look at the process and the management system instead of blaming the people. If somebody “forgot,” how do we create or improve the standardized work to help them not forget? Do we make it more clear exactly who is supposed to check and refill those dispensers and when?
“Hold people accountable” means “blame them” far too often.
What do you mean by “accountability?” I hope you’re suggesting that’s actually a management problem, not an employee problem.
What would your advice be to a manager in this situation?
I think having two dispensers only decreases the frequency with which you will run out. There is no more additional motivation to fill a dispenser.
The flag idea is good, but could be applied by the manufacture to automatically indicate when a dispenser has only 20% remaining. How about an audible alarm like a smoke alarm with a low battery?
What about finding some motivation for the staff to refill them?
Two dispensers won’t help if you still have a bad process and, I’ll add, bad leadership.
If the problem truly is “unmotivated staff,” how do you propose solving that?
In my experience, the problems are more likely things like a bad process, which includes a lack of clear responsibility for who checks the dispensers and who refills them at what frequency.
I was at a clinic today where every dispenser had some sanitizer there. I asked the manager how they accomplished that and she said there was one person with clear responsibility for that job. When everybody is responsible, nobody is.
Another thought prompted by that visit today…
One alternative to the two-bin dispenser would be somebody checking the dispensers daily. If a container of gel/foam was emptied on average every 10 days (the usage has got to be pretty consistent one would hope), you just put them on a schedule. Check them every day (which doesn’t take long) and if there’s only about 10% left, go ahead and swap it out.
I’d rather waste a little bit of sanitizer than risk infections and the cost that comes from that.
Keep in mind that the fire codes in some jurisdictions limit how much sanitizer can be placed in an area and some will even specify how far apart the dispensers must be. Touch base with your Fire Safety folks before placing big orders of dispensers
Great point. That would have to be researched and taken into account.
Hi,
I hospital I previously worked for successfully implemented a “twinbin” system (http://twinbin.com/products/the-twinbin/) where by when the lower compartment was empty a lever would be pulled to release the stock above down into the accessible bin, this would automatically raise a flag and create a clear visual control for restocking – maybe you could use that with gel being released once the lower bag was empty?
I like that concept. I wonder how to experiment with that or adapt it for hand sanitizer? That’s the right concept… have two containers/bags not just one.
I was at a hospital recently that had two dispensers side by side in one area. This was by no means the standard throughout the hospital.
The problem with this approach is that they could both get emptied at the same rate. I still think the idea of a cover or something that enforces the discipline of a two-bin system would be a nice addition… empty one bottle, and then use the other while waiting for the replacement cycle on the empty.
It’s not rocket science.