TL;DR: Small Kaizen in a Japanese Hospital Pharmacy
A visit to a Japanese hospital pharmacy shows how small, low-cost Kaizen improvements–led by frontline staff–can dramatically improve safety, efficiency, and patient experience. By using TQM, PDCA, time studies, and simple “before and after” Kaizen sheets, the pharmacy reduced walking, cut medication preparation time by 60%, lowered inventory by about 50%, and nearly doubled patient education at discharge. The lesson: continuous improvement doesn't require big projects or technology–just engaged people, good data, and leadership support.
Visiting a Japanese Hospital Known for Small Kaizen
Today, I'd like to share some highlights from one organization we visited, Seki Chuo Hospital, which is located outside of Nagoya. I have visited this hospital in 2012 and 2014 and it's interesting to see how their approach to Total Quality Management (TQM), Lean, and Kaizen has progressed and evolved. I mentioned them in a 2014 post about “quality circles.”
How a Hospital Pharmacy Applies TQM, Lean, and Kaizen
One part of our visit was an opportunity to visit the pharmacy and to hear a presentation by one of the pharmacists.
“We practice TQM,”
she said, which reminds me of the phrase “Practicing Lean” that I like. Many of these organizations in Japan would say they have been practicing TQM for 20 or 30 years. They didn't implement TQM. They never finished improving.
Scroll down for a translation of that news article that's in the slide…
Their mission is “safe and comfortable medication management.”
At Seki Chuo, the pharmacy was the first department to start with TQM in 2004.
Defining Problems as the Gap Between Current and Ideal
She framed the gap between their Ideal Status (“what we want or need to do”) and the Current Status. This gap represents the problem, which is the way I hear former Toyota people explain a problem statement.

Using PDCA, Standard Work, and Kaizen to Improve Pharmacy Work
The overview of their TQM approach emphasizes the need for Kaizen and Kaikaku (innovation). Using Plan-Do-Check-Act (PDCA) cycles, they “standardize the work” to “maintain the current level” but they are also, at times, “dissatisfied with the current status” so they “change the way it is done today.”
The hospital works to improve in the context of strategy and a “balanced scorecard,” with strategic themes and metrics in areas of finance, customer, work process, and learning and growth.
Understanding the Current State Through Observation and Data
Their “first step” is understanding the current situation to identify:
- What they want to do more of
- What they want to do less of (“asking why time is being consumed”)
They do this through time study, process mapping, and observation, to “grasp the current status.”
“We were like a mouse running all around the pharmacy.”
Then, they work to analyze the factors that lead to the gap. The next step is to implement countermeasures, such as moving medicines so there is less walking.
Results from Small Kaizen in the Pharmacy
Through “an accumulation of small Kaizen,” they reduced the amount of time required to prepare, inspect, and “cart set” a medication by 60%, as expressed in a before-and-after bar chart.
The percentage of patients getting medication instruction information at the time of discharge increased from 45.6% in 2015 to 92.6% in 2016.
The number of medication instructions was also shown as a run chart, which I always appreciate seeing, for better context.
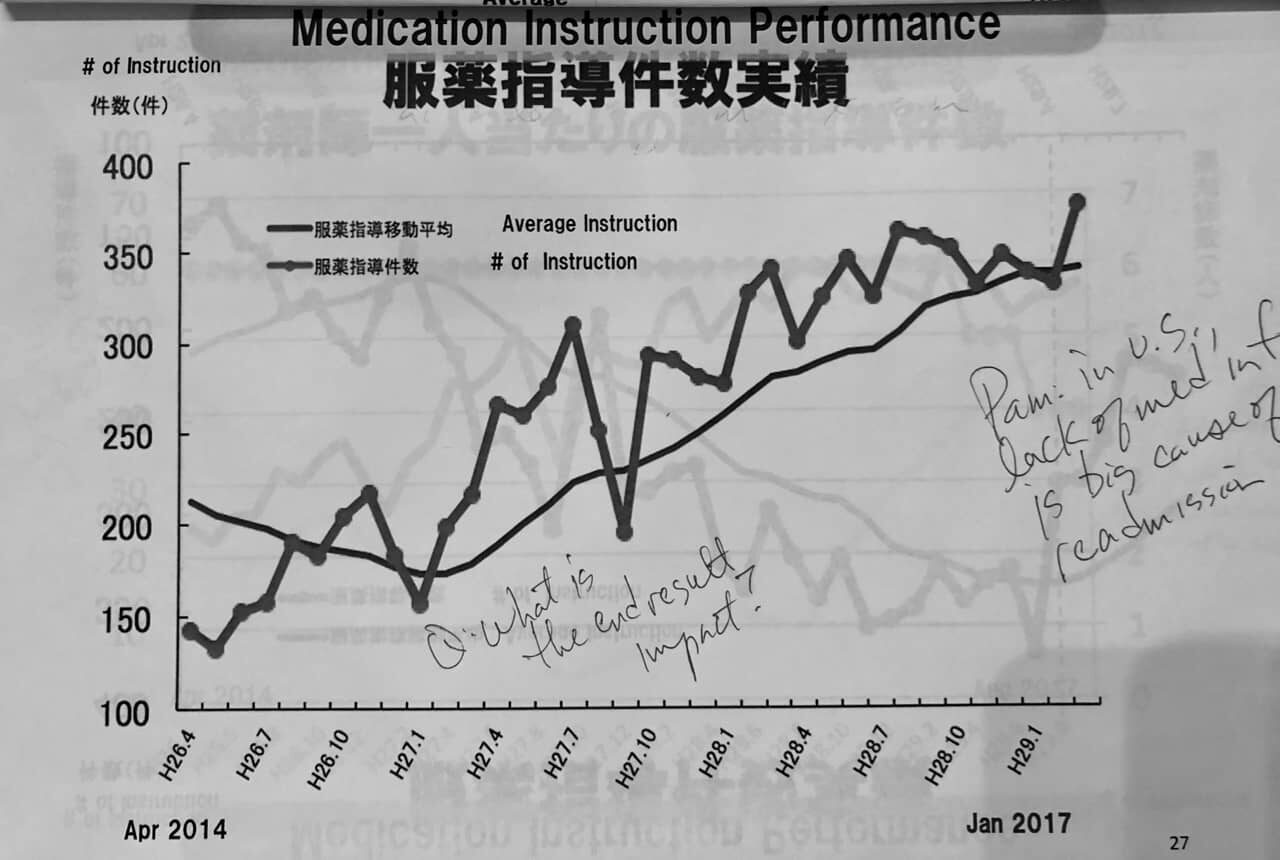
Also, through “many small changes,” inventory was reduced over a few years by about 50%, or about 6 million yen (about $55,000).
In her description of 2018 learnings, she presented that:
“We were able to discover the 3M (mura / muri / muda = irregularity / strain / waste) to be improved, by understanding the work flow by process flow chart, and visualizing the time, movement, and motion that affect the work.
All members were able to accept Kaizen activities via data visualizing, and realize that it contributes to the P&L, hence the hospital's policy achievement.”
Connecting Frontline Kaizen to Strategy and Metrics
Notice how they are connecting local improvement to strategy and measures.
When “the workplace was activated by Kaizen activities, they improved the safety and accuracy of medication deliveries, which allows them to:
“rediscover what the pharmacists really should be.”
A Patient-Centric Kaizen Example from a QC Circle
At Seki Central Hospital, staff members formed a Quality Control (QC) circle to look for practical ways to improve daily life for patients. Rather than waiting for a big project or expensive new equipment, the team focused on simple, low-cost ideas that could make a difference right away. One of their improvements was creating a newspaper stand out of cardboard so patients could comfortably read while resting. What might sound small was actually a big success: patients appreciated the convenience, and staff saw firsthand how a thoughtful change could improve the experience of care.
- These low-cost, creative solutions were well received by both patients and staff.
This is a great example of Kaizen in action — engaging frontline staff to identify problems, test solutions, and implement improvements that add value for patients. It shows how continuous improvement is less about flashy technology and more about cultivating a mindset of experimentation and teamwork. When employees feel empowered to try out their ideas, even something as modest as a cardboard stand can become a symbol of creativity, collaboration, and respect for people.
In short, the article highlights how simple, creative improvements–born from staff collaboration–helped improve patient comfort and satisfaction at the hospital.
Images
- Top photo: A patient using the cardboard newspaper stand.
- Bottom photo: Hospital staff members (including a nurse and physician) involved in the QC circle, smiling while discussing their work.
Encouraging Small Kaizen Through Contests and Recognition
Don't you love the graphics for the “small kaizen contest?”

What is a “small Kaizen?” They say it's:
“To improve / change the current way of working.”
She also compared TQM and the “Quality Circle stories” with Kaizen, saying:
“The QC story takes a long time… Kaizen is faster.”
Documenting and Sharing Kaizen with Simple One-Page Sheets
To document completed Kaizens, they use a “before and after” Kaizen template that's very similar to what Joe Swartz and I share in Healthcare Kaizen (and there's English templates available on our website).
The template includes places to write a:
- Theme
- Current condition
- “There was a problem” is how Google translates that box to the right
- Result

The cartoon woman is singing “Kaizen Sheet!”
For their 11th annual event/contest, the hospital set up a contest with five categories:
- Patient centric
- 5S
- Cost reduction
- Work improvement
- Other
And there were three “special awards” determined by the Hospital Director (CEO), an Honorary Director, and the Deputy Director. There was a committee with 18 judges.
60% of the submissions were in the “improvement of the work” category because those were “easiest to change.” 16% were patient-centric, 15% were in the 5S category, and 6% were cost reduction.
Most American hospitals would emphasize cost reduction.
Examples of Small Kaizen That Improved Patient Experience
I'll share one of the winners here, in the patient-centric category.
The problem was that bedridden patients wanted to read the newspaper, and it appears the paper is quite large. So, there was a stand built to hold the paper… it can be placed on a piece of cardboard, held with a clothespin, and placed at a slight angle.

The theme was simply: “Want to read newspapers!”
What a nice, simple thing to do for patients.
Other winning Kaizens included:
- Helping patients develop a habit of washing hands before meals
- Creating a fan coil remote control
- Revising the time for face wiping of patients
- Devising a way for patients to use their elbow to press the nurse call button
As we advocate for in Healthcare Kaizen, a simple, one-page Kaizen summary can be a powerful tool for reflection, recognition, and sharing ideas. These sheets don't take much time to fill out, even if you're adding pictures (which is far easier today than it was 11 years ago, now that everybody has a camera with them).
In a follow-up post, I write about how they responded when the number of Kaizen submissions decreased… it was an opportunity to Kaizen their Kaizen process. Here is that post:
Lessons from Small Kaizen Wins in Healthcare
The story of Seki Chuo Hospital's pharmacy shows that even small, low-cost improvements can have a big impact on efficiency, safety, and patient care. By engaging staff in identifying and solving everyday problems, they've reduced waste, improved processes, and strengthened their connection to the hospital's strategic goals.
Kaizen isn't about one-time breakthroughs — it's about building a culture where everyone looks for ways to make tomorrow a little better than today. Whether you're in healthcare or another field, what “small Kaizen” could you start this week that would make work safer, easier, or more meaningful for your team?
Conclusion — Small Kaizen, Real Impact
Small Kaizen at Seki Chuo Hospital shows that meaningful improvement doesn't require large budgets, complex technology, or special programs. It starts with people who understand the work, supported by simple methods to see problems clearly, test ideas quickly, and learn from results.
By focusing on everyday work in the pharmacy, the team reduced waste, improved safety, increased patient education, and strengthened the connection between frontline improvement and organizational strategy. Just as importantly, they reinforced professional pride by helping pharmacists “rediscover what they really should be.”
The broader lesson is universal: when leaders create the conditions for small, frequent improvements–and take them seriously–Kaizen becomes part of daily work, not an extra task. Over time, those small changes add up to better care, better work, and a stronger culture of continuous improvement.
Your Turn:
Have you seen or led a small Kaizen that made a surprising difference? Share your example in the comments — your story might inspire someone else to start their own improvement.










Nice to see that even the Japanese Pharmaceutical companies have applied the Japanese styles of production that are famous around the globe. TQM, Kaizen and Lean production methods are no doubt the best methods invented by Japanese manufacturing business to increase the efficiency of the production.