I saw this headline the other day: “U.S. Soldiers Get Just Four Hours of Ebola Training“
The phrase “just four hours” implies that it wasn't enough. How do we know? Maybe four hours of training, done properly, is all that's needed.
It might also be four hours MORE than the amount of training given to nurses, physicians, and other hospital staff.
From an article that talks about THR Presbyterian hiring a P.R. firm (!!!):
Dr. Daniel Varga, the chief clinical officer for the parent company that oversees Texas Health Presbyterian Dallas, was out front Friday in a new public relations offensive to restore trust after missteps in handling the nation's first Ebola case.
Lesson for other hospitals – it's better to not violate or destroy trust to begin with. That's true for any of us in the workplace or in our personal relations with friends and family.
This #PresbyProud campaign looks like a “grass roots initiative” but it looks like what they call “astroturfing” when a PR firm gins up people to do things that look like an organic movement. It's possible to be #NurseProud in a sincere and loving way, while being ashamed of the organization.
A picture from CNN:
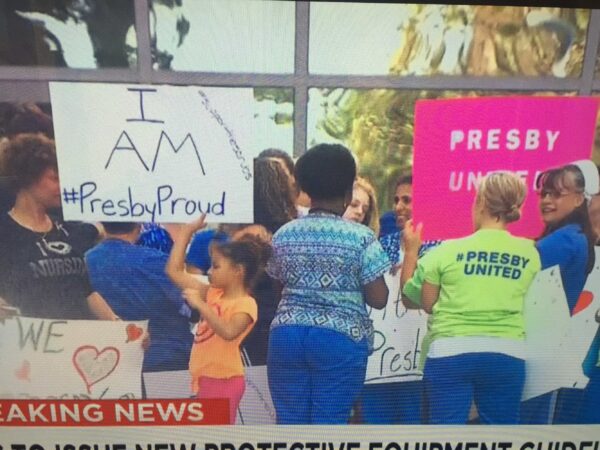
More from the article:
Varga said he believes the hospital “did do a good job of communicating and disseminating information. Where we fell short was in actually taking that through the next iteration and going through training, simulation, reinforcement.”
Information and creating awareness is, at best, the first step in effective training. That's been known since the 1940s with American manufacturers (and hospitals) used the Training Within Industry program to properly train all of the new workers that came into those workplaces. The TWI methodology is something I've used in hospitals, as have others (including Virginia Mason Medical Center) in a recent resurgence of focusing on basic “blocking and tackling” that creates an effective organization.
In the TWI methodology, we learn it's not effective to just throw a procedure at somebody.
As I heard on CNN the other night, you don't teach a kid to swim by throwing them into the pool after either showing him a PowerPoint or having him watch a YouTube video of Michael Phelps.
TWI shows us how to train EFFECTIVELY. In a nutshell, you:
- Put the student at ease (maybe hard to do when there are fears about Ebola)
- Find out what the student already knows
- Read through the written job instruction sheet with them
- DEMONSTRATE how something is done (such as properly putting on a removing personal protective equipment)
- Explain “key points” and “reasons why” you do certain things a certain way
- Have the student TRY doing it themselves
- Have the student TRY again, while explaining back the key points
It's the instructors role to ENSURE that the student not only understands, but can DO things the right way. You continue teaching until you're certain they get it. Healthcare and nursing has a tradition of “see one, do one, teach one.” One isn't always the right number.
A good instructor FOLLOWS UP to make sure the student has retained the learning and the ability to do something over time. Good training needs to be followed by good supervision.
Here's an example of what good TWI-based training looks like (from one of my hospital lab projects). You see the instructor and the student. It's one-on-one. It's detailed. It helps confirm that the learning has taken place. It's time consuming, but I don't know of any better way.

When I hear from friends or colleagues about their hospitals' Ebola prep, I hear a lot about education and awareness. I don't hear about practice.
I can be AWARE of how to do something, but it doesn't mean I can DO it.
Back to the military. What did they get in “just” four hours of training?
A team of two can train as many as 50 personnel over that four-hour time frame, USAMRIID told The Daily Beast. The training includes hands-on instruction on how to put on, remove, and decontaminate personal protective equipment, followed by a practical test to ensure that soldiers understand the procedures.
“All training is tiered to the level of risk each person may encounter,” said USAMRIID spokeswoman Caree Vander Linden.
That sounds far better than most hospital training. They “just get shown a video” or “just get a memo?”
Briana Aguirre, an ER nurse at Presby said the preparation, communication, and supplies were lack (as was the response from leadership when she asked questions).
Visit NBCNews.com for breaking news, world news, and news about the economy
That video describes at least ten process failures and leadership failures. A VP said he would get back to Briana with an answer to her questions and he never called her back.
Briana said that there was a (very) optional 30-minute seminar on Ebola prep. When they needed somebody to care for Nina Pham, they asked the nurses who had the proper training (figuring out who would care for her) and nobody put their hand up. Briana volunteered to care for her anyway.
Why would Briana lie about any of this?A cynic might think she is lying and making up stories because she's secretly a union organizer (since the National Nurses United union has been outspoken here). Some might throw that accusation at her. I wouldn't. I trust that she was put in a bad position and was a hero for 1) doing the best she could and 2) speaking out.
The problems she describes are common problems. Everyday problems that we see in most hospitals.
I feel a lot of empathy for the individual staff. For the hospital leaders there at THR Presby, not so much.
The only empathy I have is that it was, in a way, BAD LUCK that Thomas Eric Duncan came there. Similar things would have probably happened had he gone to another hospital or another health system.
THR, in their PR efforts, has released two videos.
They claim the hospital is safe and there aren't any problems. Either these staff have been put up to lying… I can understand their worry for their jobs. They might be in denial about how unsafe hospitals can be. It's what former Toyota employee Pascal Dennis always refers to as “happy talk.” Happy talk sounds good, but it interferes with real improvement.
These videos are slick… they're too slick. If lots of people can make their own “Ice Bucket Challenge” video, I'd expect to see nurses make their own simple #PresbyProud videos on their own. This is a PR campaign. Does that really rebuild trust?
As ABC reports:
To weather the storm, the hospital will need to convince people that Texas Health Presbyterian is still a safe hospital, said Dr. Dan Varga, the chief clinical officer of Texas Health Resources, which owns the Dallas hospital.
“I would tell this community that Presby is an absolutely safe hospital to come to,” Varga told ABC News chief health and medical editor Dr. Richard Besser on Thursday.
No hospital is “absolutely safe.” That's a lie… or at best it's misguided PR spin. Comments like that don't restore any of my lost trust.
Are Briana and another staff member quoted here lying about Duncan's infected trash being piled up to the ceiling in a hallway with a lot of traffic? Probably not.
“Virus-infected stuff was piling up there,” she said. “It was a reservoir.”
The hospital claims, somehow, “it went “above and beyond” national guidelines on waste.” Maybe the national standards on Ebola waste are terrible??
I'm no PR firm, but my advice to the hospital would be:
- Be humble and contrite
- Be open and honest about what happened and what didn't happen
- Talk about what you WILL do to protect staff and patients
That would help restore trust. That would also help other hospitals better prepare… not just for a possible Ebola patient, but in general.
When you look at the data about patient safety, you see that medical harm is the third leading cause of death. Thankfully, some organizations are using Lean methods to make dramatic improvements.
THR isn't an unusually bad hospital. They don't deserve to be shunned forever and they shouldn't be shut down. They need to improve. We all need to improve.
The problem at THR wasn't bad nurses or bad doctors. As usual, it's about systems and leadership. The systems failed at THR. It seems like the leadership continues to fail. And that's a “preventable management error.”









Apparently, part of the PR campaign now includes a guy who works for the Texas Hospital Association attacking me as being a supporter of “big labor,” for some strange reason.
He kept on the offensive for quite a while. See more.
I don’t see anything in this blog post supporting “big labor. Kind of makes one wonder where the fear of unionization is coming from.
Yeah, nothing I’ve said here or on Twitter should be construed as me thinking a union is a great idea.
It’s funny, when I wrote about the Lean healthcare controversy in Saskatchewan, I was attacked by labor leaders who basically said I was a management apologist and a union buster.
I guess people see what they want to see.
If I’m making both “sides” mad, then I’m either doing something right as an independent thinker, or I’m just an idiot.
If THR ends up with a union, it won’t be because of me. It will be because of the usual reasons people choose to unionize. Texas is such a strong “right to work” state, I’m surprised that:
1) The Texas Hospital Association even brought it up
2) That they chose to attack me and slander me rather than addressing the real issues
I guess that’s how PR works?
An open letter from THR:
http://www.texashealth.org/images/letter-to-the-community-101914.jpg
They admit failings in training and preparation, but they also claim to have followed CDC guidelines and that stories and allegations in the news are not true.
However, the CDC itself said (or speculated) that there were breaches in protocol.
The U.S. military is well known for the quality of its training. They take raw recruits, frequently folks who barely pass high school, and using “see one, do one, teach one” style training in every aspect of their work. Turn over is much higher than industry (four year tours) so they’re doing this non-stop. And they train until qualified, not just by goo g through the motions.
Great point. Effective organizations (and government regulatory bodies) ensure they’ve done a good job of training people, rather than blaming individuals and saying “well, we trained you!” after the fact.
The Army calls it “training to standard, not time.” Each task has a specific standard that the Soldier is expected to achieve in order to gain mastery. A long time ago, the Army used to train “to time.” Somewhere along the way, someone realized that that was not the best way to train.
With regard to Presbyterian, I would think it would be fairly easy to find out if they are as good and as safe as they claim they are: just need to look at data that talks about hospital acquired infections (very protocol driven). I am willing to bet they aren’t nearly as safe as they claim to be. You are absolutely right that this is simply a full-blown PR campaign to address what appears (from their perspective) to be an attack regarding their mishandling of the Ebola patient.
With regard to backing Unions, it is interesting that pointing to Unions as a source of cost increases in health care rather than wasteful health care delivery points out the true cognitive dissonance.
You can find their HAI rate from last year right on the Medicare website (filter by state and hospital or city): https://data.medicare.gov/Hospital-Compare/Healthcare-Associated-Infections-Hospital/77hc-ibv8
That site is harder to use than the first version of Healthcare.gov…
What conclusions did you draw from trying to filter and sift through that, Carrie?
#MarkIsBeingLazy
For Texas Presby in Dallas: CAUTIs (catheter associated urinary tract infections) are worse than the national benchmark, so there’s definitely some room to improve there. Since that’s not really a communicable infection (UTIs are usually caused by bacteria from the patient’s own body) it isn’t like how Ebola spreads. It does apply to protocols, though. Bacteria can be introduced to the bladder via the catheter by improper technique inserting it and by leaving it in too long.
For MRSA and C.diff (which are more like Ebola as far as being transmitted between patients), they are no different than the national benchmark which to me still says “room for improvement”.
They are better than the national benchmark on CLABSI (central line-associated blood stream infections) and no different than the national benchmark on surgical site infections.
Final conclusion… they are far from perfect as far as infection control goes.
#CarrieIsLazyTooButInADifferentWay
Mark,
There was an utterly brilliant presentation by Dr. Ed Chaplin at the Deming Institute meeting this past weekend on the topic of “Deming, Neuroscience and Blaming the front-line worker”. I wrote about it in my blog, but you might want to also check out this short video clip: http://youtu.be/K335makju6c
I am looking forward to getting the complete video from the Deming Institute, along with many other great videos.
Mike
From today’s paper:
“Cook Children’s prepares unit to handle Ebola virus”
Another hospital relying on videos. Education is not the same as proper training.
I hope that works.
If the nurses originally just had a video, there WERE later some nurses from Emory who came to help:
http://news.emory.edu/stories/2014/10/ehc_nurses_in_texas/campus.html
Nina Pham was diagnosed on October 12. That Emory release is from October 15.
Maybe I was cynical about the #PresbyProud PR campaign for good reasons.
Nina Pham, the RN who first contracted Ebola claims the hospital used her:
http://res.dallasnews.com/interactives/nina-pham/
Her lawsuit claims they violated her privacy, among other claims.