Hear Mark read this post — subscribe to Lean Blog Audio
Recently, I heard a friend tell another something to the effect of, “Well, if you need an MRI, the new hospital out by Alliance will do one for $XXX cash out of pocket, especially if you're willing to go at 6 am.”
I forget the exact number, but it was a number that was lower than this person's insurance co-pay and out-of-pocket cost. It made them think about what they should do (saving money is good, but it wouldn't go toward their annual deductible).
This article caught my eye over the weekend:
From the article:
“When Cheryl Millican found out she needed surgery, her Dallas-based doctor told her it would cost roughly $38,000 out of pocket.”
That's the out-of-pocket amount even WITH health insurance.
Millican learned, from a friend, that she could drive three hours up to Oklahoma and get the same procedure for $8,000… by paying cash.
“A number of specialists — oncologists, physical therapists, and even some hospitals — are jumping on board as well.”
In the Lean approach, we say “value is defined by the customer” based on the problem you need solved or the job you need accomplished. Just because something costs five times as much doesn't mean that it's providing five times the value.
And, in healthcare, people have learned that higher cost doesn't mean higher quality. If anything, lower prices indicate better quality because it's a sign that waste has been eliminated from the process. The same types of waste that lead to quality risk are usually similar or correlated with the waste that increases cost. Efficient medicine is safe medicine?
Organizations like the Surgery Center of Oklahoma post prices on their website. There's transparency. That allows patients to make better choices, right?
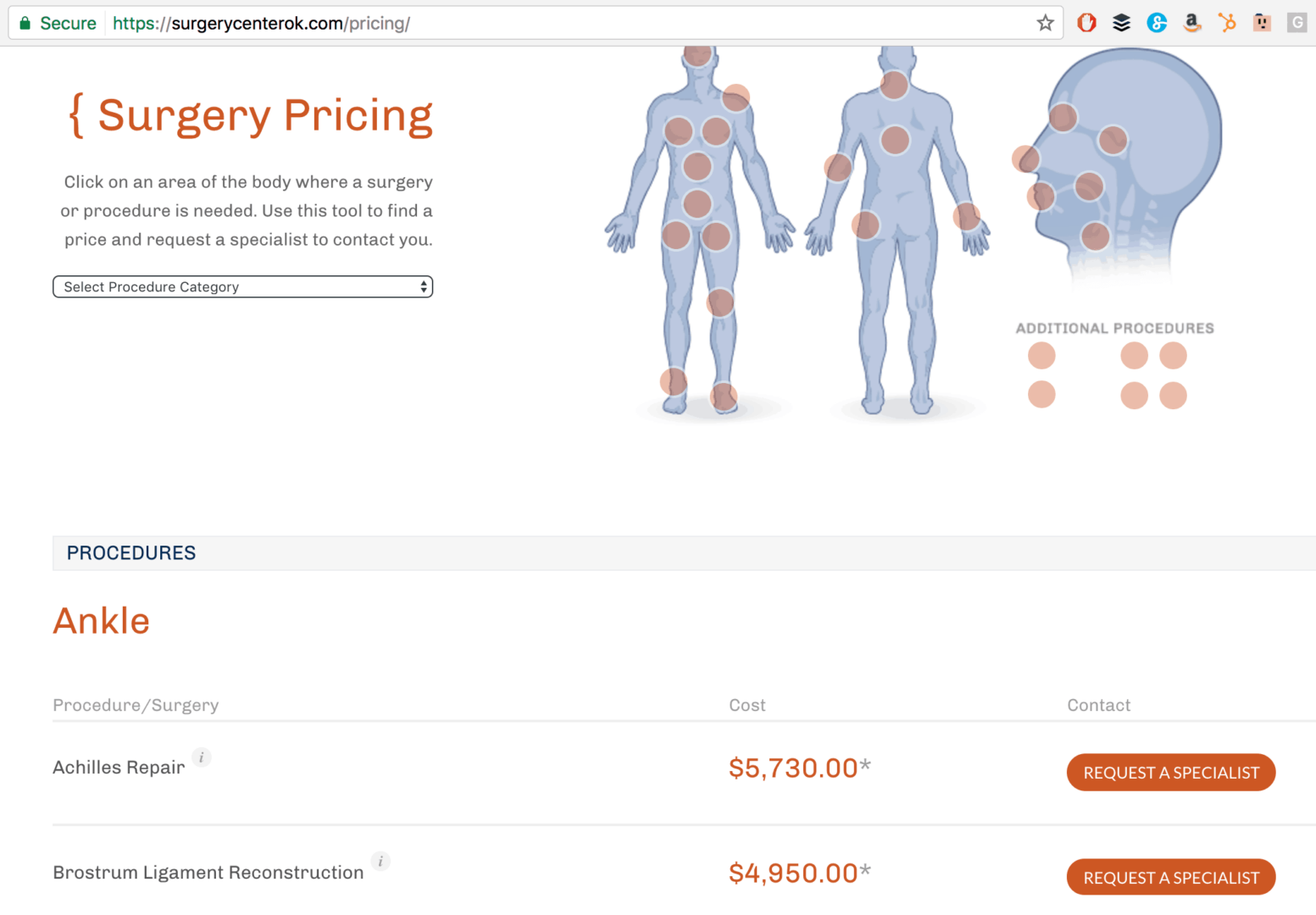
There's a long list of procedures and prices on that page.
It says, on the surgical center's site:
“Fees for the surgeon, anesthesiologist and facility are all included in one low price. There are no hidden costs, charges or surprises.”
The surprise charges in healthcare often upset people… for example, they learn that the surgeon and the hospital are “in-network,” but the anesthesiologist was not.
Price isn't the only thing that matters in the value equation… so does quality:
“The site also discloses information about its infection rates, and relies heavily on reviews.”
Their FAQ page has the infection rates and more information.
“Wherever you decide to have your surgery, you should inquire about the rate of infection in their facility. Our infection rate for 2015 was .008%. Listed below is our infection summary over the last 10 years:
2015 .008%
2013 .13%
2012 .015%
2011 .05%
2010 .001%
2009 .001%
2008 0.4%
2007 0.2%
2006 0.3%These percentages have been and remain astoundingly low compared with an estimated national average of 2.6 % per year.”
The 2014 data is missing I'll assume that's just an oversight. It's good that they provide the context of the national average, otherwise their infection rates might not mean much to a patient.
You'd be disappointed in me if I didn't visualize that data in a line chart, right? I've also added the surgical center's average infection rate as I calculated it (the average of the annual numbers):
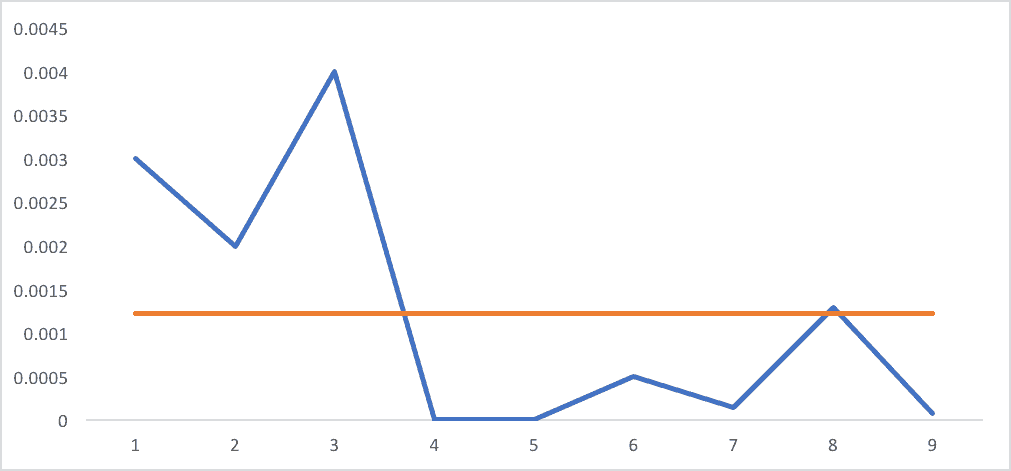
Are infection rates decreasing? Or fluctuating around an average? It's hard to know for sure with just that many data points.
Are other surgical centers doing this? Again, from the article:
“The [Free Market Medical Association] lists 67 providers that disclose their prices, including other surgery centers, imaging centers, and a handful of physical therapy practices among specialties. And Freedman said she adds about 9 to 10 new providers every month to the FMMA's search tool.”
So, the patient pays less (good), has a lower risk of infection (good), and the physician also gets paid more (good for them):
“Because the Surgery Center's price for a hysterectomy was so much lower than what Millican had been quoted at a Dallas hospital, she asked her doctor why he chose to do the procedure at a lower price. He told her frankly that it was profitable for him. When he performs the procedure using insurance, he is paid $500, she recalled him telling her. For her procedure, he told her, he got paid five times that.”
Employers who are “self insured” are increasingly sending patients around the country for domestic medical tourism. John Torinus and his company Serigraph have been doing that, as we discussed in episode #192 of my podcast. Employers like Wal-Mart and Lowes are sending patients to Virginia Mason Medical Center for better value care.
It seems like the only one who loses in this equation is the health insurance company.
What do you think of the idea of researching providers and traveling a bit to get better care at a lower price? Is this a trend? Or are some of these providers an outlier?
If you work for a big traditional health system, how will your organization respond to this competitive threat? What are they doing now? How can Lean help provide better quality, better service, and lower prices?
What do you think? Please scroll down (or click) to post a comment. Or please share the post with your thoughts on LinkedIn – and follow me or connect with me there.
Did you like this post? Make sure you don't miss a post or podcast — Subscribe to get notified about posts via email daily or weekly.
Check out my latest book, The Mistakes That Make Us: Cultivating a Culture of Learning and Innovation:









Mark,
This was a very insightful blog post. We will continue to see price and quality transparency impact consumer decisionmaking.