Mark's note: Ankit Patel is a returning guest blogger and a good friend in the world of Lean and Lean Healthcare. Check out his blog and website.
By Ankit Patel:
 In all my years of practicing lean/process improvement I've noticed one thing, the technical elements are easy but the people change is hard. Mark wrote about change management a couple of weeks ago and talked about how there needs to be less change management and more change and I wanted to share with you a model for change that's been tested and works very well.
In all my years of practicing lean/process improvement I've noticed one thing, the technical elements are easy but the people change is hard. Mark wrote about change management a couple of weeks ago and talked about how there needs to be less change management and more change and I wanted to share with you a model for change that's been tested and works very well.
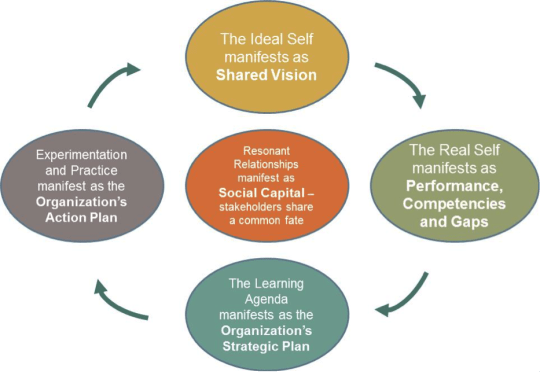
I wrote about some elements of the change process a few weeks back in a post I titled Climbing the Mountain of Change where I listed some of the elements to look for in a successful change process. I want to introduce to you the Intentional Change Theory Model and an example of a successful change and an unsuccessful change. The model was created by Richard Boyatizis and is a based on 30 years of field research of what works. Originally, the model was for individuals and the organizational level change model was developed after by Richard Boyatzis and Ellen VanOosteen. There are other models that also work and I like this model because of its foundation on emotional intelligence and the comprehensiveness of the system. Here is the model:
Case:
I did a project at the Cath Lab at a hospital and their concern was around there being too much overtime. We had a brand new manager who was promoted from the internal ranks of the cath lab (Jane), an administrator who is getting pressured about performance (John), a new head doctor for the cath lab (Dr. Doe). After sitting down with the steering committee team of Jane, John, and Dr. Doe we decided to do a Kaizen event around the process between the operations, or in other words a change over time reduction. We would then take the results of the kaizen and roll it out to the rest of the team. We are going to take a look at two parts of the project, the Kaizen portion which was successful and the roll out portion where the change wasn't so successful.
Part I: Kaizen
The kaizen was a 2 day blitz on improving the current state of the changeover process. The event was successful in its objective.
The team:
- Jane
- Dr. Doe
- Three cath lab employees which Jane has worked with before
- One cardiac Fellow
- Myself and another facilitator
Objective:
Reduce changeover time by 40% from 52 min to 32 min.
Outcome:
By the end of the kaizen we meet our objective and the team was performing at the new baseline level of 32 min.
Let's take a look at the change model to see why it was so effective.
Shared vision: This was a bit tricky to create because not all the team members initially agreed that the goal was necessary. We did this in a couple of ways. First we presented the business case for reducing the time down, that wasn't enough so we decided to take a video of the current process with the team members that were in the Kaizen. Once they saw the variation in their work they seemed to agree on next steps and agreed to a shared vision of improving the changeover process from 52 min to 32 min by standardizing the work of everyone team member.
Performance Gaps and Competencies: This is the standard current state evaluation process that you would do in any kaizen event. We did a current state map and a future state map to determine what we wanted to keep, what we wanted to change, and what we wanted to improve.
Strategic plan/learning agenda: This was another natural part of the kaizen process where we deployed a plan to test the improvements and then roll out the improvements post kaizen event.
Action Plan/experimenting: This was the part of the event when we did our iterations with the new processes and tweaked our process.
Social Capital: This covers a large range of things. We have a language around the new processes. We had a report out to the leaders, doctors, and nurses who could attend. The leaders who were in the event were very resonant during the event. This means that during the event Jane and Dr. Doe exhibited high emotional intelligence and were in tune with the direction the team needed to go. John the administrator also created a great amount of buzz around the output of the event to the rest of his peers and team.
Because we have all of these factors we were able to effectively create a solution with the team in the event.
Part II: Roll out to the rest of the organization
This portion of the project was not as successful and we were not able to rollout the improvements through the whole lab.
Team:
The entire cath lab – doctors, techs, nurses, and administration.
Objective:
Rollout the standard work and process improvements to every team in the cath lab.
Outcome:
Let's take a look at where we fell short without the changes in the kaizen being able to stick and continue.
Shared vision: This was the biggest area we fell short. There wasn't a common vision from one person to the next let alone from doctors to techs to nurses. Everyone seemed to have their own priorities. This coupled with all the other changes going on caused major pushback from the nurses and techs.
Performance Gaps/Competencies: We decided to take a look at the different teams and where they stood currently. We saw some teams had more room for improvement vs. others and saw that there may need to be unique approaches to those teams. Where we didn't do a good job was doing analysis on the leadership's ability to make the change happen. I will say that it is my opinion that if we had a solid shared vision that was agreed upon by everyone then the change would have been much easier for the leadership to implement the change.
Strategic plan/learning agenda: We took the information we had about the teams and decided to implement a rollout strategy and a daily meeting process to help facilitate learning the new process.
Action plan/experimenting: We had daily meetings, individual coaching, team coaching, audits, and peer coaching all available for implementation.
Social Capital: This is another area where we fell short in our change effort. We didn't educate the entire cath lab on the language and we tried doing prizes and rewarding good behavior but those efforts never stuck. They didn't stick primarily because the leadership was not resonant during this process. This was not the fault of leadership; they were tasked with many things at once and were a little overwhelmed with the amount of other work that needed to be done. They were in what's called sacrifice syndrome. It's when you get to the point where the leadership stress makes you an in effective leader until you can pull yourself from the sacrifice syndrome.
The primary items that took us away from our goal were no shared vision and very little to no social capital for the change. If I were to do it again I would actually address a shared vision for the entire cath lab first before tackling the individual events. Techniques like Appreciative Inquiry are great tools to help develop shared vision among groups. The other thing I would have done was to take a look at the timeline and see how much the leaders could help to implement the change. When we were doing the changes it was a bit too much for the leadership to deliver.
There are many details left out and I would love to hear from you all on your thoughts.
Thanks,
Ankit
BIO: Ankit is a senior consultant at The Lean Way Consulting and combines his Lean/Six Sigma background with organizational development. He's done work with large manufacturers as well as large health systems. You can find more about Ankit at www.TheLeanWayConsulting.com.
What do you think? Please scroll down (or click) to post a comment. Or please share the post with your thoughts on LinkedIn – and follow me or connect with me there.
Did you like this post? Make sure you don't miss a post or podcast — Subscribe to get notified about posts via email daily or weekly.
Check out my latest book, The Mistakes That Make Us: Cultivating a Culture of Learning and Innovation:




![No More Flavor of the Month! Learn How To Deliver Sustainable Change [Webinar Recording]](https://www.leanblog.org/wp-content/uploads/2023/11/lean-blog-lynn-kelley-webinar-preview-change-238x178.jpg)




Excellent. Many of us talk about the diffculties of change, but not in the level of detail that this case study presents. Thank you.
I’m glad you like it Dean.
Thank you Mark for letting me post on your blog.
Thanks,
Ankit